What is Vitiligo?
Understanding the Condition

UNDERSTANDING VITILGO
What is Vitiligo?
Vitiligo is a long-term skin condition where pigment-producing cells (melanocytes) stop functioning, causing white patches to appear on the skin.
What is Vitiligo?
Vitiligo causes loss of skin colour in patches, resulting in the area looking white or pink in appearance. Hair in body parts affected by vitiligo may also turn white or grey. It can affect any part of the body and varies from person to person.
Key facts about vitiligo:
It is non-contagious.
Vitiligo cannot be passed from one person to another through touch, contact, or any form of interaction. It is entirely safe to be around someone with vitiligo.
It is an autoimmune-related condition
Light therapy exposes your skin to a type of ultraviolet (UV) light, which may restore your natural skin color
It can affect skin, hair, and mucous membranes
Vitiligo is most visible on the skin, but it can also cause whitening of the hair, eyebrows, and eyelashes, as well as affect the inside of the mouth and other mucous membranes.
It progresses over time
Vitiligo patches may grow larger, new patches may appear, and the condition can change over months or years. These changes vary widely between individuals.
While vitiligo is not physically harmful, it can impact confidence and quality of life. Understanding how it works, what causes it, and how it can be managed is key to living with the condition.
Take our short self-assessment quiz to understand how vitiligo may be impacting your quality of life
What Causes Vitiligo?
Vitiligo occurs when melanocytes, the cells responsible for producing skin pigment, are destroyed or stop working. The exact reason this happens is not fully understood, but researchers believe several factors are involved:
Autoimmune factors
Vitiligo can happen when the body’s immune system mistakenly attacks and destroys its own melanocytes. This is similar to how the immune system behaves in conditions like type 1 diabetes. People with vitiligo are also more likely to have other autoimmune conditions.
Genetic factors
Vitiligo can run in families. If a parent or sibling has vitiligo, your risk of developing it is higher. Researchers have identified several genes associated with the condition, though having these genes does not guarantee you will develop vitiligo.
Other Triggers
In some people, vitiligo appears or worsens following a specific trigger. Common triggers include:
- Emotional or physical stress, such as illness, bereavement, or major life events
- Skin injuries from sunburn, cuts, or trauma to the skin
- Chemical exposure from certain industrial chemicals
- Hormonal changes, including puberty or pregnancy
These triggers alone do not cause vitiligo, but they may activate it in people who are already genetically predisposed.
Understanding what may have triggered your vitiligo is a helpful first step. Speaking with a dermatologist can help you identify patterns and build a management plan that works for you.

What are the Different Types of Vitiligo?
There are two main types of vitiligo, non-segmental and segmental vitiligo. The most common is the non-segmental type, wherein symptoms typically appear as symmetrical white patches on both sides of the body. Segmental vitiligo is much less common, with white patches appearing on only one segment or side of the body.
Non-segmental vitiligo (generalised)
This is the most common type. Patches appear symmetrically on both sides of the body, for example, on both hands, both knees, or both sides of the face. It tends to spread gradually over time and is strongly linked to autoimmune activity.
Segmental vitiligo
Segmental vitiligo affects only one side or segment of the body. It tends to progress more rapidly for one to two years, then stabilise. It is less commonly associated with autoimmune conditions and can respond well to certain treatments.
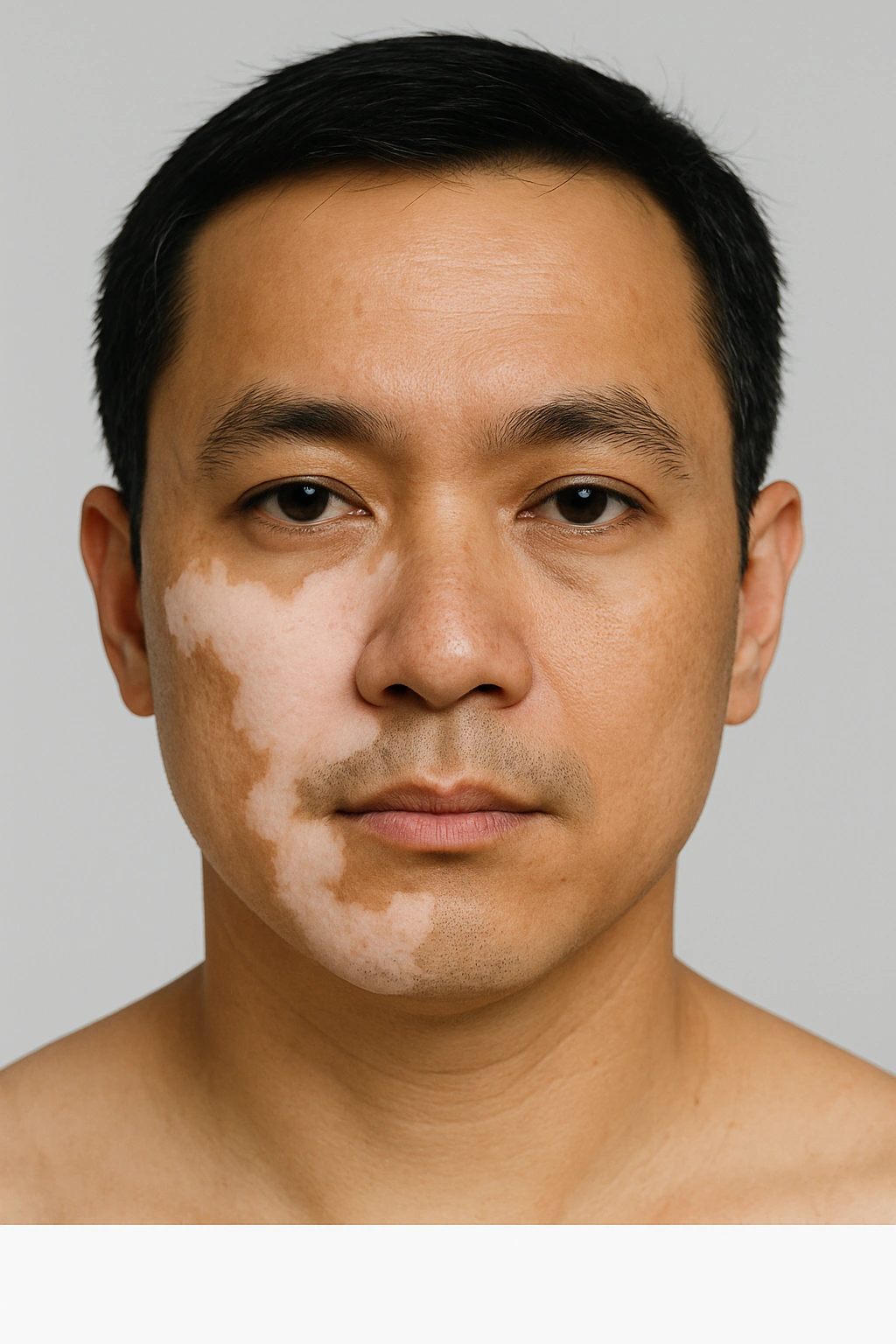
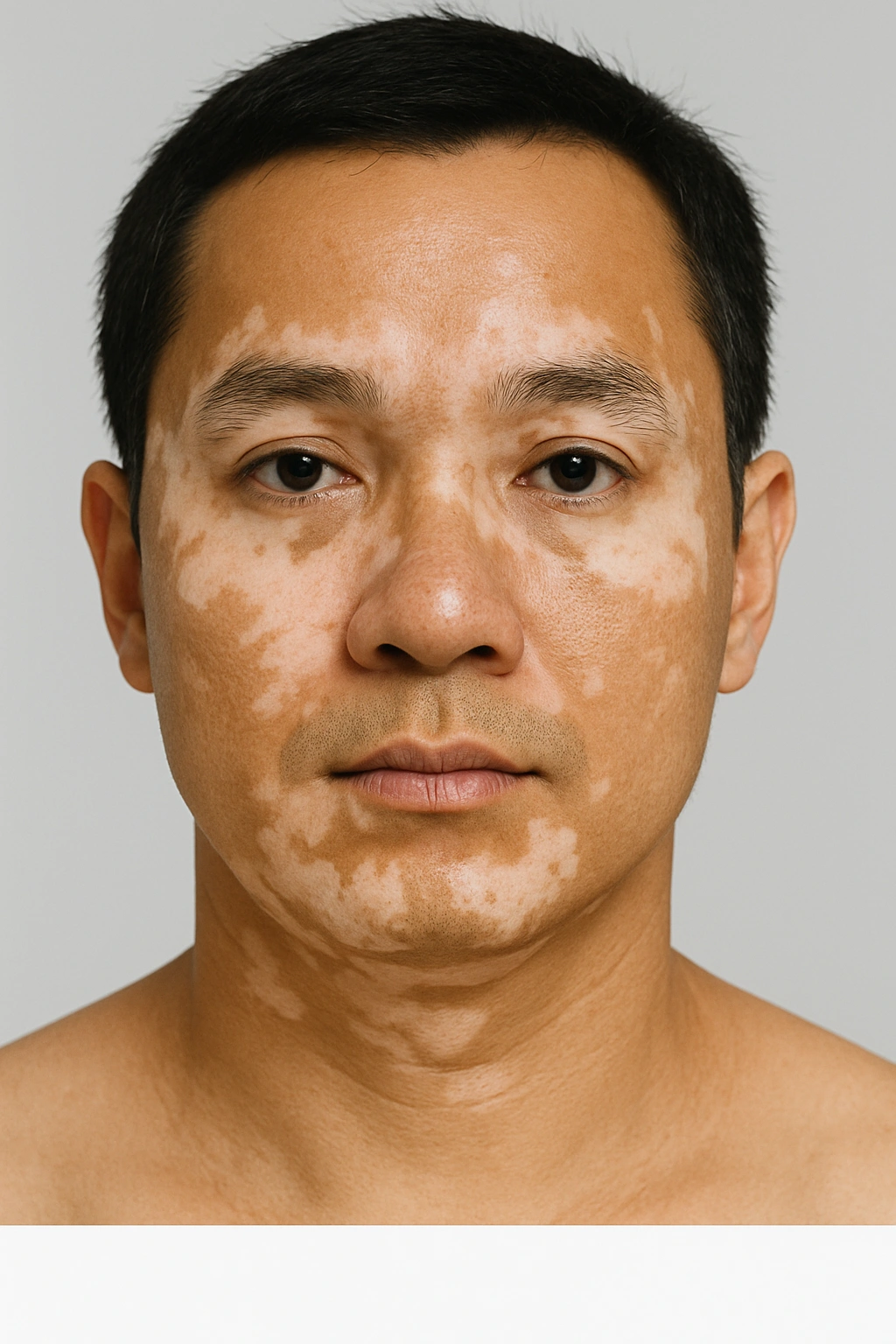
Focal vitiligo
This refers to one or a few patches in a localised area that do not spread in the typical pattern of non-segmental vitiligo. It may evolve into one of the above types over time.
Universal vitiligo
A rare form where pigment loss covers more than 80% of the body. It is most commonly seen in people with longstanding, widespread non-segmental vitiligo.
Mucosal vitiligo
This type affects the mucous membranes, such as the lips, gums, and inside of the mouth. It may appear alongside skin involvement or on its own.
Not sure which type of vitiligo you have?
Common Areas Affected by Vitiligo
Vitiligo can appear anywhere on the body, but certain areas are more commonly affected than others.
- Face, around the eyes, mouth, and nose
- Hands and wrists, including the knuckles and fingers
- Feet and ankles
- Armpits and groin, areas where skin meets skin
- Genitalia
- Inside the mouth
- Hair on the scalp, eyebrows, eyelashes, or beard
Vitiligo patches may start small and gradually grow, or remain stable for years. The pattern varies widely between individuals.

Often one of the first areas where vitiligo appears, especially on knuckles and fingers.
Vitiligo may spread along the forearms and elbows in noticeable patterns.
Frequently affects areas around the eyes, mouth, and forehead.
Can cause loss of pigment inside the mouth, lips, or nose.
Patches commonly form around toes, ankles, and the tops of the feet.
How is Vitiligo Diagnosed?
Vitiligo is usually diagnosed through a physical examination or various medical tests.
Clinical examination
A dermatologist will examine the size, shape, and location of depigmented patches. The pattern and distribution of patches help determine the presence and type of vitiligo. Your doctor will also ask about your personal and family medical history.
Wood's lamp examination
A Wood’s lamp is a handheld ultraviolet (UV) light used in a darkened room to examine the skin, hair, and scalp for different medical conditions. Under the lamp, vitiligo patches glow bright white or blue-white, making them easier to identify. This quick and painless tool helps doctors confirm the diagnosis and assess the extent of depigmentation.
Biopsy
In some cases, a skin biopsy may be taken to confirm the absence of melanocytes. A small sample of depigmented skin is sent to a laboratory for analysis. A biopsy is not always necessary, but it can be useful when the diagnosis is uncertain or to rule out other conditions.
Blood tests
Because vitiligo is associated with other autoimmune conditions, your doctor may recommend blood tests to check thyroid function, blood glucose levels, and other markers. Early detection of related conditions allows for better overall management.
When should you see a skin specialist?
You should see a dermatologist if you notice new white or pale patches on your skin, particularly if they are growing or spreading. Early diagnosis of vitiligo means treatment can be started sooner, which may help slow progression and improve outcomes.
If you are noticing changes in your skin and are unsure whether it is vitiligo, do not wait. Early diagnosis gives you more options for treatment and support.
Treatment and Management of Vitiligo
Vitiligo is typically not harmful to your health. However, different medical treatments may help slow its progression, promote repigmentation, and potentially restore skin colour.
Topical treatments
Topical corticosteroids and calcineurin inhibitors are applied directly to affected skin. They work by suppressing the immune response. These are often the first line of treatment for vitiligo, particularly for small or newly developed patches.
Light therapy (phototherapy)
Narrowband ultraviolet B (NB-UVB) phototherapy is one of the most effective treatments for vitiligo. It involves exposing the skin to controlled UVB light, usually 2-3 times per week. Results appear gradually over several months, with the therapy showing best results for face and neck area.
Surgical options
Surgery may be considered for stable vitiligo that has not responded to other therapies. Options include skin grafting and melanocyte transplantation, where healthy melanocytes are taken from unaffected skin and transplanted to depigmented areas.
Depigmentation
For people with extensive vitiligo affecting most of the body, depigmentation of remaining pigmented skin may be an option. This involves removing the remaining colour to create a more uniform skin tone. It is a permanent process and is considered only when vitiligo is very widespread.
The Repigmentation Process
Repigmentation is the process by which skin colour returns to depigmented areas in those affected by vitiligo. It can happen naturally or as a result of treatment, and the pattern of return varies from person to person.

Depigmentation

Repigmentation
How repigmentation occurs
Repigmentation begins when surviving melanocytes are stimulated to migrate and produce pigment again. This process is gradual and can take months. It often starts as small pigmented dots within a patch before spreading outward.
What affects repigmentation
Several factors influence how well and how quickly repigmentation occurs:
- Duration of vitiligo. Newer patches tend to respond better than older ones
- Location. The face and trunk typically respond better than the hands and feet
- Hair follicle involvement. Patches with white hair may have fewer surviving melanocytes
- Treatment type and consistency
- Individual variation in immune response

Managing expectations
Repigmentation for vitiligo can be slow and inconsistent. Most people see partial improvement, but some patches may not respond to treatment at all. It is important to maintain realistic expectations and to continue your treatment consistently for the best results.
Connecting with others who understand the vitiligo journey can make a real difference. Learn more about our vitiligo support group here.
Have Questions About Vitiligo?
Frequently Asked Questions
Living with vitiligo can come with uncertainty, especially if you’re newly diagnosed or supporting someone who has it. This FAQ section is here to help you better understand the condition, how to care for your skin, and where to find support.
What is the main cause of vitiligo?
The main cause of vitiligo is an autoimmune reaction. In this case, the body’s immune system mistakenly attacks and destroys melanocytes, the cells responsible for producing skin pigment. When melanocytes are damaged or destroyed, the skin loses its colour in those areas, resulting in white or pale patches.
Certain genes linked to immune function have been associated with a higher risk of developing the condition. People with vitiligo are also more likely to have other autoimmune conditions, such as thyroid disease or type 1 diabetes.
What are the early signs of vitiligo?
The earliest sign of vitiligo is usually a small, pale or white patch on your skin that appears lighter than the surrounding area. These early patches often develop on sun-exposed areas such as the face, hands, forearms, or around the eyes and mouth.
The edges of the patch may be slightly irregular, and the area may gradually become fully depigmented over time. Some people notice premature whitening or greying of hair in the affected area, including the scalp, eyebrows, or eyelashes.
The patches themselves are not painful or itchy, which means they can sometimes go unnoticed or be dismissed initially. If you observe any unexplained loss of skin colour, it is worth consulting a dermatologist early, as prompt treatment generally yields better results.
Can vitiligo spread?
Yes, vitiligo can spread across the body. However, the pattern and rate of spreading are different for each person. New patches may appear on different parts of the body, and existing patches can gradually grow larger over time.
Non-segmental vitiligo, the most common type, tends to be more likely to spread than segmental vitiligo, which often stabilises after an initial period of progression. Treatment can help slow or halt the spread in some cases, particularly when started early. Regular monitoring by a dermatologist is important to track any changes and adjust treatment accordingly.
Is vitiligo permanent?
Vitiligo is considered a long-term condition, but it is not always permanent. Some people experience natural repigmentation, where colour gradually returns to affected areas without any treatment.
Many others achieve significant pigment return through medical treatments such as phototherapy, topical medications, or newer therapies like JAK inhibitors.
The likelihood of repigmentation depends on several factors, including the type of vitiligo, how long patches have been present, and their location on the body. It is important to have realistic expectations. Full, even repigmentation is not always achievable, but meaningful improvement is possible for many people.
Can vitiligo be cured?
There is currently no definitive cure for vitiligo. However, this does not mean the condition cannot be effectively managed. With the right treatment, many people achieve significant repigmentation and are able to control the progression of the condition.
Research into the underlying causes of vitiligo is ongoing, and new treatment options, such as JAK inhibitors, are emerging as understanding of the condition improves. For some people, vitiligo may go into a period of stability where it does not actively spread.
What triggers vitiligo?
Vitiligo can be triggered by stress and hormonal changes in people who are already genetically susceptible to the condition.
Emotional stress is one of the most commonly reported triggers. Periods of anxiety, grief, or major life changes can precede the onset or flare-up of the condition. Physical stress on the skin, such as sunburn, injuries, and chemical exposure, can also trigger new patches.
Hormonal changes during puberty or pregnancy may also play a role in triggering the condition in some individuals. It is important to note that triggers do not cause vitiligo on their own, but only activate it in people who already have an underlying predisposition.
Does stress cause vitiligo?
Stress does not directly cause vitiligo. However, both emotional and physical stress are among the most commonly reported triggers for the onset or worsening of the condition.
Stress is thought to affect the immune system in ways that may increase autoimmune activity, which could explain its connection to vitiligo. Managing stress will not cure vitiligo, but it may help reduce the likelihood of flare-ups.
Strategies such as regular exercise, mindfulness, adequate sleep, and talking therapies can all support stress management. Connecting with a support group can also help, as the emotional burden of living with vitiligo itself can become a source of stress.
Is vitiligo genetic?
Vitiligo has a clear genetic component. Around 20–30% of people with vitiligo have at least one close family member who also has the condition, suggesting that genetic factors play a significant role.
Researchers have identified several genes associated with vitiligo, many of which are linked to immune system function and the regulation of melanocytes. However, having these genes does not guarantee that a person will develop vitiligo/
If you have a family history of vitiligo or other autoimmune conditions, your risk may be higher than average. Being aware of this risk can help you monitor your skin and seek advice early if you notice any changes.
Can diet affect vitiligo?
There is currently limited clinical evidence that diet directly affects vitiligo. Nevertheless, specific foods can play a supporting role in overall skin and immune health.
A balanced diet rich in antioxidants, found in fruits, vegetables, and whole grains, may help support the immune system and reduce oxidative stress, which is thought to contribute to melanocyte damage.
While you should only take supplements under medical guidance, ensuring adequate intake of these nutrients through your daily diet is generally beneficial.
Is vitiligo dangerous?
Vitiligo is not dangerous or life-threatening. It does not cause physical pain, is not contagious, and does not affect the body’s internal organs or overall physical health.
However, there are some health considerations that people with vitiligo should be aware of. Depigmented skin lacks melanin, which means it has no natural protection against UV radiation and is much more prone to sunburn.
This makes sunscreen and protective clothing essential, particularly in Singapore’s year-round sun.
Vitiligo is also associated with a higher risk of other autoimmune conditions, such as thyroid disorders, type 1 diabetes, and alopecia areata, so regular health check-ups are advisable.
Can children develop vitiligo?
Yes, vitiligo can develop at any age, including in early childhood. Around half of all cases are first diagnosed before the age of 20.
The condition behaves similarly in children as it does in adults, though the emotional impact during formative years can be particularly significant. Children with vitiligo may face teasing, questions from peers, or feelings of being different, which can affect their confidence and social development.
Age-appropriate psychological support, alongside medical treatment, is an important part of managing vitiligo in children.
Is vitiligo more common in certain skin types?
No, vitiligo affects people of all skin types, ethnicities, and backgrounds in roughly equal proportions globally.
However, the visibility of vitiligo can differ significantly depending on skin tone. On darker skin tones, depigmented patches can appear highly visible. In Singapore and across Southeast Asia, where many people have medium to deeper skin tones, this contrast can be particularly noticeable.
Regardless of skin tone, the underlying condition is the same, and treatment options are equally applicable. It is important that all individuals with vitiligo, regardless of their skin type, have access to appropriate medical care and emotional support.
